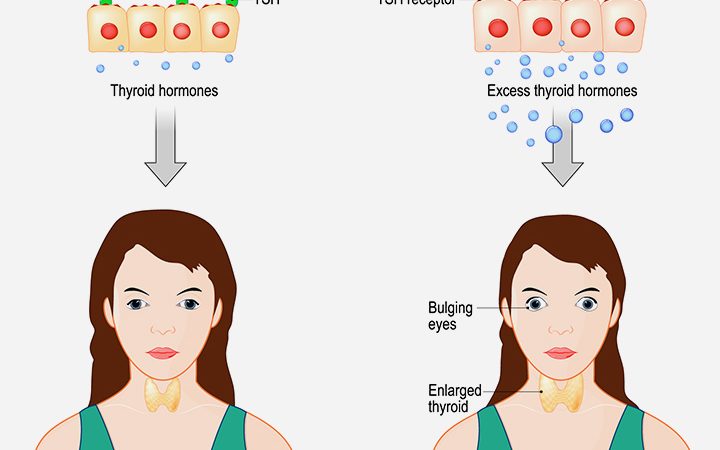
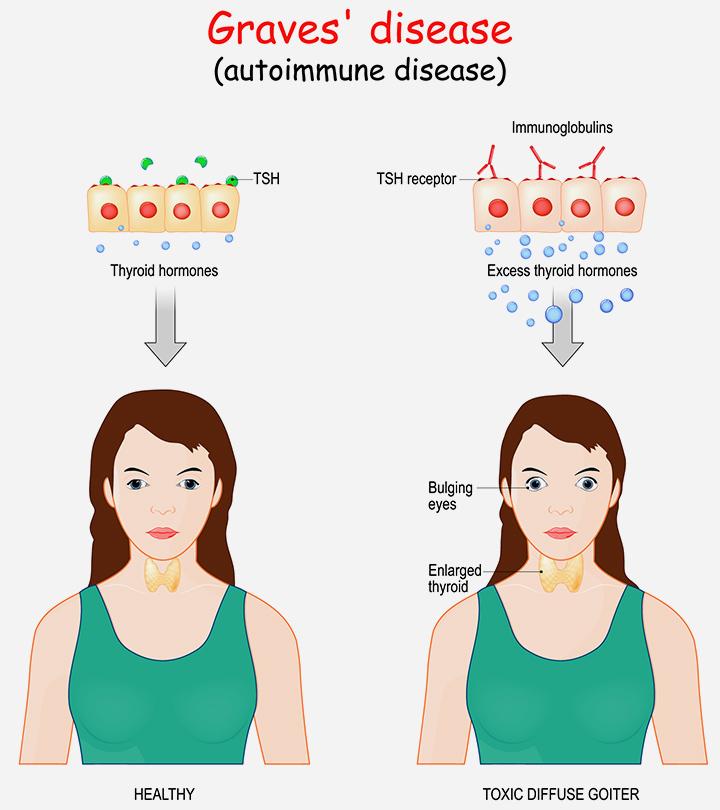
Graves’ disease (GD) is a thyroid disorder and accounts for 10-15% of thyroid disorders in children and teens (1). It is a chronic autoimmune disease where problems with the body’s immune system lead to the condition. Graves’ disease is the most common cause of hyperthyroidism in children. Children with Graves’ disease have a loss in body weight, rapid heartbeats, fatigue, and other issues that need long-term management (2).
Read more about the causes, symptoms, diagnosis, and treatment options for Graves’ disease in children.
What Causes Graves’ Disease In Children?
The exact cause of Graves’ disease remains unclear, but it is believed that the disease is caused due to genetic and environmental factors. The pathophysiology of the disease is based on the binding of an antibody called thyroid-stimulating immunoglobulin (TSI) to the thyroid-stimulating hormone (TSH), signaling an increased synthesis of thyroid hormones, T3 and T4, and growth in the thyroid gland (overactive thyroid). It eventually leads to hyperthyroidism (3).
Studies suggest that alterations in several genes (the majority of them belonging to the HLA complex) increase a person’s overall risk of developing this disease (4). In addition, genes involved in thyroid function (thyroglobulin (Tg) or the thyroid-stimulating hormone receptor (TSHR) genes) and modification of immune responses (such as CD25, CD40, CTLA-4, and FOXP3 genes) are also linked to the development of Graves’ disease (5).
What Are The Risk Factors For Graves’ Disease?
Children are more at risk of developing Graves’ disease if they (6) (7):
- Have a family history of thyroid disorders
- Have a family history of autoimmune conditions
- Are female and are nearing puberty (puberty marks hormonal changes)
- Consume abnormal amounts of iodine through diet or medications
- Are subjected to chronic stress
- Have a history of viral or bacterial infections
- Have chromosomal abnormalities such as Down’s syndrome or Turner syndrome
- Have the habit of smoking
What Are The Symptoms Of Graves’ Disease In Children?
The symptoms of Graves’ disease may vary among children. However, the most common signs of this condition are (6) (7):
- Swelling around the neck
- Difficulty in swallowing
- Rapid heartbeats
- Increased blood pressure
- Trouble sleeping
- Weight loss, despite a good appetite
- Excess sweating
- Shaking of hands and legs, nervousness
- Protruding eyes
- Chronic fatigue and weakness
- Hyperactivity and irritability
- Frequent mood swings
- Poor concentration
- Hair loss, especially around the scalp
- Sensitivity to cold
- Frequent urination and bedwetting
- Changes in menstrual cycle in girls
- Frequent feelings of being emotionally low, crying, or yelling
- Slow growth rate, leading to short height
The symptoms of Graves’ disease may resemble other health conditions seen in children. Consult a doctor if you notice any signs in your child for appropriate diagnosis and definite treatment.
How Is Graves’ Disease Diagnosed In A Child?
Experts suggest that a combination of physical examination, a detailed study of a patient’s history, and specific lab tests are essential for diagnosing Graves’ disease in children. Your child’s doctor may suggest the following tests (8).
- Physical examination: It helps detect signs of restlessness, tremors, abnormal heart rates, bulged eyes, and blood pressure abnormalities.
- Blood tests: A series of blood tests are done to measure the levels of T3, T4, and thyroid-stimulating hormones. Additional blood tests may also be done to check the TSI antibody levels.
- Ultrasound: An ultrasound is used to detect an enlarged thyroid gland and increased blood circulation in the thyroid gland.
- Radioactive Iodine uptake scan: This is an additional test used when the lab tests and scan cannot confirm the diagnosis. The test helps in determining iodine absorption by the thyroid gland.
How Is Graves’ Disease In Children Treated?
The treatment for Graves’ disease in children will depend on the age, the severity of symptoms, medical history, and overall health status of the child. Your child’s doctor may consider the following treatment options (1).
- Antithyroid medications: Antithyroid drugs are used as initial treatment for Graves’ disease in children. Remission is achieved in most children after treatment with antithyroid drug therapy. These drugs are known to suppress the synthesis of thyroid hormones. The most commonly used drugs are carbimazole, propylthiouracil, and methimazole.
- Radioactive iodine: Radioactive iodine therapy is effective if your child has serious side effects from medicines. The low-dose iodine therapy aims at preventing the recurrence of Graves’ disease.
- Thyroidectomy: This is a surgery indicated in children who don’t respond to medications or radioactive iodine therapy. Surgery is an option only in serious cases as there is a possibility of acute to serious complications, such as hemorrhage, after the surgery.
Discuss with your child’s doctor the suitable therapy for your child and the guidelines to follow while monitoring your child after treatment.
What Are The Complications Of Graves’ Disease?
A common complication of Graves’ disease in children is Graves ophthalmopathy, a rare vision-threatening eye condition. In some cases, overexposure to certain treatment drugs may cause agranulocytosis, a rare bone marrow disorder leading to insufficient production of white blood cells. Untreated hyperthyroidism may lead to a rare but serious condition called thyroid storm, causing high fever and blood pressure (3) (7).
Graves’ disease is the most common cause of hyperthyroidism in children. There are no known ways to prevent the condition, but you may ensure extra care if your child is prone to the risk factors. Despite the availability of definitive treatments, there is a risk of relapse and drug-based side effects. The condition may require lifelong monitoring and management with appropriate techniques instructed by your child’s doctor.
References:
MomJunction’s articles are written after analyzing the research works of expert authors and institutions. Our references consist of resources established by authorities in their respective fields. You can learn more about the authenticity of the information we present in our editorial policy.
Recommended Articles
- Pityriasis Rosea In Children: Causes, Symptoms, And Treatment
- Neck Pain In Children: Causes, Symptoms, Remedies, And Treatment
- Nasal Polyposis In Children: Causes, Symptoms, Treatment And Prevention
- Turner Syndrome In Children: Causes, Symptoms, Treatment, And Prevention
The following two tabs change content below.