Rosacea is an uncommon, chronic skin condition in children that causes redness of the facial skin. It has flare-ups that may be more frequent and intense with time. Late diagnosis could lead to pimples, pustules, broken blood vessels, skin redness, and other skin conditions (1) (2).
Rosacea could affect any part of the face and neck and is treated depending on the symptoms. Although this non-contagious skin inflammation has no cure, some measures can help prevent the symptoms from worsening.
Read this post to learn about the diagnosis, treatment, and prevention of rosacea in children.
Is Rosacea Common In Children?
Rosacea rarely affects children and is more common in 30 to 60-year-olds. If your child has been experiencing temporary facial redness, it is more likely due to sun damage. In most cases, children with fair skin tone experience thinning of the skin due to sun damage, resulting in visible blood vessels around the cheeks (1) (3).
However, a few children may show early signs of rosacea, such as flushed skin, for long durations (4).
What Are The Causes And Risk Factors Of Rosacea In Children?
The exact cause of rosacea is unknown, but the following could be the causative factors of this chronic condition (1) (5)
- Abnormalimmune system response
- Genetic factors
- Reaction towards mites and microbial organisms
- Blood vessel disorders
- Family history of rosacea
- Fair skin
- Sun exposure
- Scandinavian or Celtic ethnicity
Further, the following factors may trigger rosacea flare-ups and irritation (1) (6) :
- Sun exposure
- Hot baths
- Spicy foods
- Extreme temperature
- Cosmetics
- Hot beverages
- Aerobic exercises
- Some medicines
What Are The Symptoms Of Rosacea In Children?
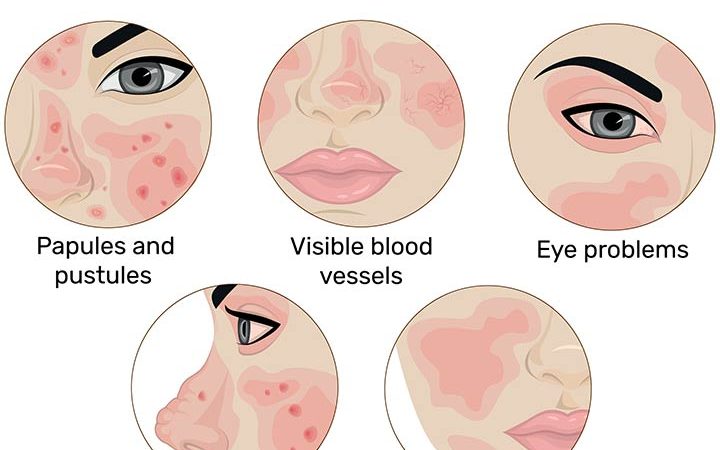
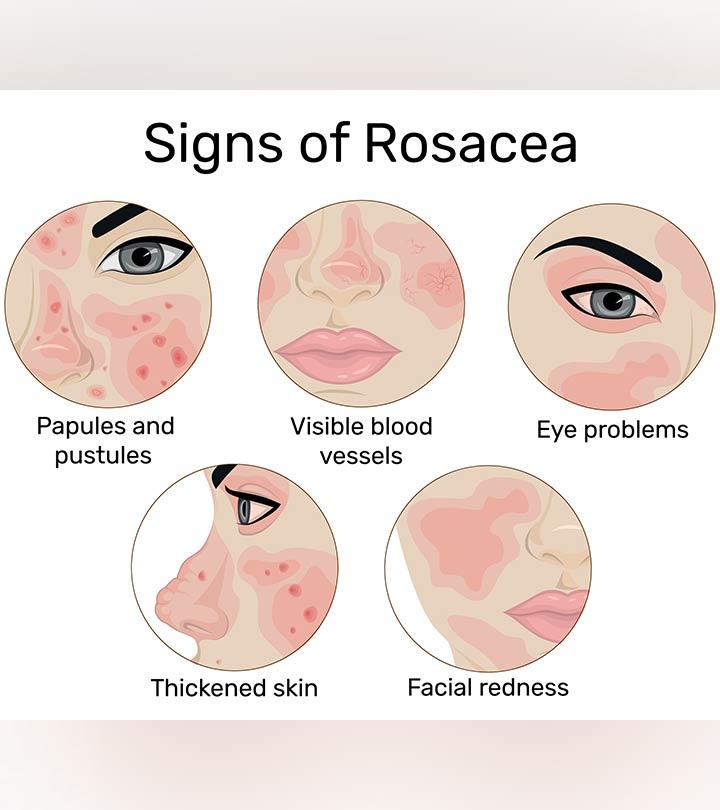
Rosacea is characterized by a series of clinical manifestations, which may vary among children. The common signs of childhood rosacea are (1) (4) (7)
- Long-lasting redness: Red flushes may appear on the cheeks, chin, nose, forehead, or neck and aggravate when in contact with a trigger. The redness may only last for a while but reappears occasionally.
- Visible blood vessels: Dilated, small blood vessels (telangiectasia) that seem webbed may appear on the face.
- Small bumps and pimples: Bumps and pustules (filled with pus) may occasionally appear in the reddened areas.
- Skin plaques: Raised patches of skin that may sting.
- Thick skin: The skin becomes tight and thick, especially around the nose (rhinophyma), giving it a bulbous appearance. It may also appear on the forehead, cheek, ears, and chin. This is not a primary symptom of rosacea but may follow the other symptoms.
- Ocular rosacea (around the eyes): Recurrent pink eye (conjunctivitis or styes (pimples on the edge of the eyelid), watery eyes, burning or stinging sensations, redness, or irritation as if there is sand in the eyes are a few signs of ocular rosacea.
What Are The Complications Of Rosacea In Children?
Untreated rosacea may result in the following complications (4) (8):
- Permanent redness on the face
- Conjunctivitis (inflammation of the eye’s outer membrane)
- Rhinophyma (bumpy and bulbous nose due to swollen nasal sebaceous glands)
- Partial or complete visual impairment due to progressed ocular manifestations of rosacea
How Is Rosacea Diagnosed In Children?
Rosacea is mostly diagnosed based on a physical examination and medical history. Occasionally, the medical care advisor may suggest blood tests to rule out the possibility of lupus (an autoimmune disease) (1) (9)
They may also try to rule out other skin conditions such as acne, periorificial dermatitis (inflammation of the skin around the mouth), or allergies (4) (10)
What Is The Treatment For Rosacea In Children?
The treatment for childhood rosacea aims at managing the symptoms since there is no permanent cure. Your medical care supervisor may advise a combination of treatment plans for increased effectiveness. These may include (4) (11)
- Medication: Based on the symptoms, the dermatologist may suggest gels or creams. Oral antibiotic therapy or topical steroids may help reduce inflammation. Over-the-counter medications may be ineffective in treating childhood rosacea and, hence, should be avoided.
- Alternative treatment: If telangiectasia is observed, laser therapy may be advised to shrink the enlarged blood vessels. In case rosacea leads to rhinophyma, surgery of the nose may be recommended by the doctor.
How Can You Prevent And Manage Rosacea In Children?
Although your child cannot prevent the onset of rosacea, they can curb the flaring up of its symptoms. Here are some tips to help prevent rosacea in children (12) (13):
- Identify the triggers: As triggers may aggravate sensitive skin, identify and eliminate the triggers to help reduce the irritation.
- Apply sunscreen: Daily use of sunscreen is recommended. Dermatologists may suggest fragrance-free and SPF 30 sunscreens containing titanium oxide, zinc oxide, or both.
- Protect the affected area: As hot and cold temperatures may trigger rosacea, ask your child to drape a scarf in extreme conditions. Opt for silk or acrylic scarves as they may be less triggering.
- Avoid heat: Avoid hot baths and excessive clothing. Ensure they maintain distance from heat sources such as heaters, and keep a cold water bottle or cold towel handy during intense activities.
- Consume the right foods beverages: Avoid spicy foods and hot drinks. Opt for cold or room-temperature beverages instead.
- Read labels: Many cosmetics and skin care products contain ingredients that may trigger rosacea, such as sodium lauryl sulfate (common in shampoos and toothpaste), alcohol, camphor, or menthol.
- Subtle skin care: Choose a gentle skincare routine for your child. Use a gentle cleanser on their face and pat it dry. Avoid scrubbing or massaging their face, and use products recommended by your dermatologist.
- Perform patch tests: Always perform a patch test for new products to check if they cause any reactions.
- Moisturize: Studies show that moisturizing the skin, whether oily or dry, with a prescribed product could be helpful.
With a few lifestyle changes and the right treatment, the complications of rosacea in children can be prevented. If your child frequently has redness or pimples on the face, get them checked for rosacea. Ensure to note down all your child’s symptoms to help your doctor make a correct diagnosis.
References:
MomJunction’s articles are written after analyzing the research works of expert authors and institutions. Our references consist of resources established by authorities in their respective fields. You can learn more about the authenticity of the information we present in our editorial policy.
Recommended Articles
The following two tabs change content below.